Emanuelle Vieira Do Nascimento1, Livia Alves Peçanha Rios1, Nathalia Silveira Finck2*
1FAESA University Center, Undergraduate Student in Dentistry (FAESA)
2FAESA University Center, Professor in the Undergraduate Dentistry Program
Abstract
This study aimed to map the main signs and symptoms, diagnostic criteria, and conservative interventions for temporomandibular disorder (TMD) in children up to 12 years old, emphasizing the importance of multidisciplinary care. It is a scoping review conducted according to PRISMA-ScR guidelines, using the PCC strategy. The search was performed in the PubMed and Google Scholar databases, in Portuguese and English, covering the period from 2015 to 2025, and included classic studies. The searches were carried out on October 4, 2025. Two independent reviewers selected the articles using Rayyan, and disagreements were resolved by a third evaluator. From 97 records, with no duplicates removed, 97 were screened, 18 were read in full, and 16 studies were included. The studies showed heterogeneity in methodological designs and diagnostic criteria. The prevalence of TMD varied according to the methods used, with the pediatric DC/TMD criteria being the most frequently applied. The most common manifestations were orofacial pain, headache, joint noises, and functional limitation. Conservative interventions—such as pain education, occlusal splint use, physical therapy, cognitive-behavioral therapy, and speech therapy- showed favorable outcomes in pain reduction and functional improvement, with a low occurrence of adverse events. It was concluded that TMD in children is a multifactorial condition requiring age-appropriate diagnosis. Conservative and interdisciplinary management should be prioritized, avoiding irreversible procedures. Further standardized and prospective studies specific to the pediatric population are needed.
Keywords: Temporomandibular Joint Disorders; Child; Interdisciplinary Approach; Orofacial Pain
Introduction
Temporomandibular disorders (TMD) comprise muscular, skeletal, and neuromuscular alterations that affect the temporomandibular joint and associated structures [16]. Although well documented in adults, TMD in children remains underdiagnosed, despite its impact on eating, sleep, speech, and emotional well-being [12]. Early diagnosis through questionnaires, clinical examination, and imaging tests, combined with multidisciplinary treatment, is essential to prevent complications and promote conservative approaches [10].
In this context, early intervention associated with a multidisciplinary approach can prevent long-term complications related to craniofacial growth, resulting in significant improvements in the child’s quality of life [9].
The relevance of this research is justified by the fact that TMD, although often associated with adults, also affects children, impacting growth and the development of essential functions, which may lead to emotional difficulties and negatively affect school performance. For these reasons, early identification is crucial to prevent severe complications and to enable conservative treatments, which are less invasive and effective [12].
Furthermore, investigating risk factors, symptoms, and treatment options is fundamental to improving diagnosis and the quality of life of affected children, highlighting the importance of a multidisciplinary approach in managing this condition.
Therefore, the objective of this study was to analyze, highlight, and raise awareness of the signs and symptoms of TMD in children in order to facilitate early diagnosis and, consequently, identify the most appropriate treatment.
Methodology
This study was conducted in accordance with the PRISMA-ScR guidelines (Preferred Reporting Items for Systematic Reviews and Meta-Analyses extension for Scoping Reviews), prioritizing transparency and methodological rigor. The corresponding checklist is included as supplementary material.
To formulate the guiding research question, the PCC strategy (Population–Concept–Context) was applied:
1. Population (P): children up to 12 years of age presenting signs or symptoms of temporomandibular disorders (TMD).
2. Concept (C): diagnostic and/or treatment methods for TMD, with a focus on conservative and multidisciplinary approaches.
3. Context (C): different healthcare settings (primary, secondary, or tertiary care), with no restriction regarding the clinical environment.
Searches were conducted in the PubMed and Google Scholar databases (gray literature), including articles published between 2015 and 2025, as well as classic studies considered relevant. In Google Scholar, the practical screening was based on the first 100 results. No restrictions were imposed regarding study design, provided that the studies addressed the diagnosis and/or treatment of TMD in children from a multidisciplinary perspective. The search strategy was developed using controlled and non-controlled descriptors, as illustrated in Table 1.
Combinations of terms were used with the Boolean operators AND/OR, including: “temporomandibular disorder”/“TMD” AND “child*”/“pediatric*” AND “diagnosis”, “screening”, “treatment”, “intervention”, “multidisciplinary*”, and “TMD prevalence”.
Table 1: Research strategy
|
Database |
Search strategy |
Languages |
Period |
|
PubMed |
("Temporomandibular Disorder*" OR "TMD" OR " Temporomandibular |
English/ |
2015–2025 (includes previous |
|
Google Academy |
("Temporomandibular Dysfunction" OR "TMD") AND ("Child*" OR "Pediátr*") |
English/ Portuguese |
2015–2025 (including grey |
Eligibility Criteria:
Inclusion:
i. studies involving children ≤12 years of age
ii. articles addressing the diagnosis and/or treatment of temporomandibular disorders (TMD)
iii. studies with a multidisciplinary approach (dentistry, physical therapy, speech-language pathology, psychology, pediatrics, rheumatology, among others).
Exclusion:
i. studies conducted exclusively with adults
ii. publications in languages other than Portuguese and English (iii)studies that do not address TMD from a multidisciplinary perspective.
Study Selection:
Records were exported to Rayyan, an online tool (https://www.rayyan.ai), for the evaluation of titles and abstracts of all included articles, considering the inclusion and exclusion criteria. Duplicate records (n = 0) and screened studies (n = 97) were assessed in two stages (titles/abstracts and full-text review) by two independent reviewers (L.A.P.R. and E.V.N.). Disagreements were resolved by a third reviewer (N.S.F.).
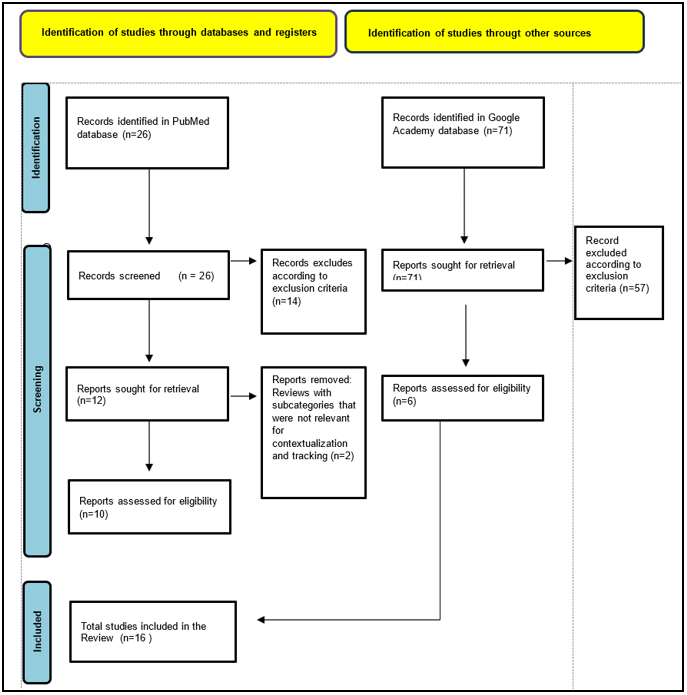
The reasons for exclusion at the full-text stage were recorded. The selection process is illustrated in a flowchart adapted from the PRISMA-ScR guidelines (Figure 1).
Data Extraction
Data collection was performed using a standardized form, recording the following information: author/year, country, study design, sample size and age range, definition/criteria for TMD, diagnostic/screening instruments, professionals involved, type of intervention (conservative/invasive), outcomes (pain, mandibular function, quality of life), follow-up duration, main results, and adverse events. Data extraction was conducted independently and subsequently verified jointly.
Results
Study Selection
From a total of 97 records identified in the PubMed and Google Scholar databases, the previously defined inclusion and exclusion criteria were applied. After the initial screening of titles and abstracts, eligible articles were subjected to full-text review.
As a result of this process, 16 articles met the criteria and were included in this review. Figure 1 presents the PRISMA-ScR–adapted flowchart, detailing the processes of identification, screening, eligibility, and inclusion of the analyzed studies.
Figure 1 – PRISMA-ScR–adapted flowchart summarizing the study identification and selection process.
The main results reported by the included studies are described in Figure 1. From a total of 97 records identified in the PubMed and Google Scholar databases, duplicate records were removed and the previously defined inclusion and exclusion criteria were applied.
After the initial screening of titles and abstracts, the eligible articles were subjected to full-text reading. As a result of this process, 16 studies met the criteria and were included in the present review. The PRISMA-ScR–adapted flowchart (Figure 1) details the process of identification, screening, eligibility, and inclusion of the studies.
The selected studies showed great methodological heterogeneity, but, taken together, they demonstrate that temporomandibular disorders (TMD) in children have a multifactorial etiology, involving biological, psychological, and behavioral aspects. The main outcomes investigated were prevalence, clinical signs and symptoms, psychosocial impact, diagnostic methods, and the effectiveness of different therapeutic approaches.
Among the included studies, the adaptation of the DC/TMD criteria for the pediatric population stood out, developed through the international Delphi study [10, 11], which resulted in adapted physical (Axis I) and psychosocial (Axis II) diagnostic instruments for children and adolescents, expanding diagnostic reliability.
The data also show that the prevalence of TMD in children ranges from 16% to 68%, depending on the diagnostic criteria and methodologies adopted [13, 8, 14]. Among the most frequently reported symptoms are orofacial pain, headache, joint sounds, tooth wear, and functional limitations, frequently associated with a negative impact on school performance and emotional well-being [12, 1].
Regarding therapeutic strategies, the literature highlights the importance of a multidisciplinary approach, involving dentistry, physiotherapy, psychology, speech therapy, and pediatrics [9]. In contrast, occlusal adjustment, once widely used, did not demonstrate significant effectiveness in the treatment or prevention of temporomandibular disorders (TMD) and is currently considered an obsolete resource or one of very restricted application [7, 15, 2]. It is important to emphasize that not all authors addressed or presented data regarding the prevention of TMD in children.
In general, the results confirm that early diagnosis and conservative and interdisciplinary management are fundamental to prevent complications, minimize the chronification of pain, and improve the quality of life of children with TMD.
Table 2 presents a synthesis of the main conservative interventions identified in the studies included in this review, highlighting the authors who mention them and the description of each approach. It is observed that the literature preferentially emphasizes non-invasive strategies, such as pain education, guidance on habits, physiotherapy, the use of occlusal splints when indicated, psychological therapies, and speech therapy. These interventions reinforce the interdisciplinary perspective and the need to consider physical, emotional, and behavioral factors in the management of TMD in children.
Table 2: Conservative interventions, authors, and description
|
Intervention |
Authors |
Description |
|
Pain education |
Rongo et al. (2021/2022); Porto et al. (2024); |
Explanation to the child and caregivers about the |
|
Education on habits / elimination |
Rongo et al. (2022); Porto et al. (2024); Bertoli et |
With speech therapy, perform functional reeducation and |
|
Correction of patterns |
Porto et al. (2024); Bertoli et al. (2009) |
With speech therapy, correct masticatory and |
|
Occlusal splint |
Porto et al. (2024) |
Intraoral device for muscle relaxation and joint |
|
Manual therapy |
Porto et al. (2024); Yost et al. (2020) |
Through physiotherapy, perform exercises, stretching, |
|
Cognitive-behavioral therapy |
Yost et al. (2020); Rongo et al. (2022) |
Psychological intervention for pain management, |
|
Sleep-related interventions |
Tapia-Sierra et al. (2025); Rongo et al. (2022) |
Improvement of sleep hygiene and management of |
Table 3 brings together the main methodological data of the selected studies, including country, objectives, mentioned forms of prevention, diagnostic methods used, and main results. The methodological diversity observed among the articles reveals the heterogeneity of the literature on temporomandibular disorders (TMD) in children, both in relation to diagnostic criteria and to the instruments employed and outcomes analyzed. Even so, the synthesis of these findings allows the identification of important trends, such as the multifactorial etiology of TMD, the relevance of early diagnosis, the role of adaptations of the pediatric DC/TMD, and the importance of integrated approaches in treatment. The organization of this information in a table facilitates comparison between studies and highlights gaps that justify the need for more standardized research directed at the pediatric population.
Table 3: Extraction of the main methodological data and results of the included studies
|
Author (year) |
Country |
Objectives |
Prevention |
Diagnosis |
Main results |
|
Carrara et al. |
Brazil |
Establish consensus in |
Guidance on signs and |
Clinical and |
40–75% of the population |
|
Bertoli et al. |
Brazil |
Evaluate TMD in children |
Guidance on signs and |
Clinical evaluation |
Multifactorial etiology |
|
Rosal & |
Brazil |
Discuss ways to diagnose |
Secondary |
Clinical examination, |
Symptoms include pain, |
|
Yost et al. (2020) |
USA |
Identify research |
Prevention based |
Recommends |
TMD with muscular, |
|
Rongo et al. |
International (Delphi) |
Adapt DC/TMD criteria |
Prevention through diagnostic standardization. |
Axis I (physical) and |
Validated criteria for |
|
Porto et al. |
Brazil |
Evaluate |
Tertiary prevention: |
Integrated |
Treatment reduces |
|
Koh & |
United |
Evaluate the effectiveness |
Practice |
Systematic |
No evidence of benefit; |
|
Tsukiyama et |
Japan/USA |
Evaluate occlusal |
— |
Review of 11 |
Did not demonstrate |
|
Clark & |
USA |
Critical review of occlusal |
— |
Evaluation of clinical |
Limited studies; occlusal |
|
Minervini et al. |
Italy |
Meta-analysis of the |
— |
Diagnosis based |
Prevalence ranges from |
|
Tipia-Sierra et |
Spain |
Associate TMD with sleep |
— |
Clinical examination, |
Relationship between |
|
Sena et al. |
Brazil |
Evaluate the prevalence of |
— |
Clinical evaluation. |
Variable prevalence; need |
|
Ekberg et al. |
International |
DC/TMD diagnostic |
Prevention |
Adaptations of the short |
Adapted instruments |
|
Engel (1977) |
USA |
Propose the |
Baseline model for |
Integrates biological, |
Supports the |
Discussion
The term temporomandibular disorders (TMD) encompasses a set of conditions that affect the temporomandibular joint, the masticatory muscles, and associated structures, with muscular and/or articular manifestations [16]. It is a broad label that includes different clinical presentations, ranging from painful conditions to functional alterations capable of compromising mastication, speech, and the patient’s well-being.
The most frequent symptoms include pain in the temporomandibular joint region, often radiating to the neck or ears, tenderness and fatigue of the masticatory muscles, otalgia, joint sounds, headache, and, in more advanced cases, limitation of mandibular movements and tooth wear. Such manifestations may affect growth and development, interfere with feeding, communication, and sleep, and impact emotional well-being, with a possible increase in anxiety and irritability [12].
According to the 1st Consensus on TMD and Orofacial Pain, between 40% and 75% of the general population presents at least one clinical sign of TMD [1]. In children, however, prevalence remains poorly defined: studies report rates ranging from 16% to 68% [13, 8, 14]. This wide range mainly results from the heterogeneity of diagnostic criteria and methodologies employed, which limits direct comparisons and data uniformity.
The international Delphi study, developed precisely to address the lack of specific diagnostic criteria for children, suggests that the occurrence of pain and other signs or symptoms related to TMD increases with age, indicating a trend toward higher prevalence as children grow older [10]. This method was developed by an international group of experts affiliated with INfORM (International Network for Orofacial Pain and Related Disorders Methodology), who, in view of the absence of standardized instruments for the pediatric age group, conducted several rounds of consensus to adapt the DC/TMD for children and adolescents. Even so, the scarcity of investigations focused exclusively on the pediatric population hinders precise epidemiological estimates for this age group.
TMD comprises a spectrum of conditions that may arise in isolation or in combination, including myalgia, myofascial pain, arthralgia, headache attributed to TMD, disc disorders, degenerative joint disease, TMJ subluxation/luxation, and overlap with other orofacial pain disorders [16].
In addition, the findings of this review align with the study by Finck et al. (2025), which identified a significant association between clinical signs related to TMD, occlusal alterations such as Class II, lip incompetence, and increased overjet, and characteristics of mouth breathers. The study showed that children with an oral breathing pattern presented a higher prevalence of musculoskeletal complaints, upper airway alterations, and a greater risk for sleep-disordered breathing, reinforcing the importance of an integrated assessment involving dentistry, otorhinolaryngology, and speech therapy. These results indicate that structural and functional facial factors may influence both mandibular mechanics and respiratory health, broadening the multifactorial understanding of TMD in childhood.
Regarding etiology, in children it is considered similar to that observed in adults [10, 3]. Multiple factors interact as initiating, predisposing, and perpetuating factors: biological aspects (TMJ development, trauma), psychological factors (stress, depression), behavioral factors (bruxism and parafunctional habits), and postural/neuromuscular factors contribute to the onset and maintenance of the condition.
Despite this multifactorial nature, for decades occlusal adjustment was adopted as the first therapeutic choice, supported by the hypothesis that occlusal interferences were the main cause of TMD. This view has been challenged. The Cochrane systematic review [7] found no robust evidence of effectiveness in treating or preventing TMD, discouraging its use as an isolated approach. Similar results were observed by Tsukiyama et al. (2001), who, after analyzing 11 clinical studies (413 participants), identified no relevant clinical benefits of occlusal adjustment compared with sham treatments or controls. [2] also pointed out recurrent methodological limitations (small samples, lack of blinding, short follow-up), compromising the validity of the findings. Thus, occlusal adjustment came to be viewed as an obsolete intervention or one of very restricted indication, always within a multidisciplinary approach and only in specific cases.
From this perspective, [10] emphasize the importance of a diagnostic process adapted for children and adolescents with TMD complaints, considering behavioral, structural, social, and psychological particularities, including differences in pain threshold compared with adults. Clinical evaluation should integrate inspection, palpation, and functional tests, complemented by imaging examinations when clinically indicated (e.g., radiographs, ultrasonography, magnetic resonance imaging). Anamnesis must be detailed, with age-adapted forms (as proposed in the Delphi study), addressing problem location, triggering and modulating factors, as well as topics such as sleep, symptoms of depression/anxiety, stress, and resilience, which are fundamental to understanding the pain experience in childhood [10]. In the pediatric Delphi, Part 1 adapted Axis I (physical criteria), with history questionnaires and clinical examination adjusted for ages 6–9 years and 10–19 years, achieving consensus ≥80% in the first round and ≥70% in subsequent rounds. Part 2 adapted Axis II (psychosocial assessment and pain-related disability), incorporating appropriate scales for depression, anxiety, catastrophizing, sleep disorders, and resilience, with consensus among experts in TMD and pain psychology. The adaptations included simplified language, use of visual pain scales, and adjustments in temporal history intervals (for example, considering complaints present for at least two weeks), increasing validity in the pediatric age group. These advances favor standardized and reliable diagnosis in young populations, facilitating multicenter research and harmonization of clinical data.
TMD is not a single condition and may have different causes, complaints vary over time and context. In this sense, the biopsychosocial model [5] stands out, highlighting the interaction of biological, psychological, and social factors in the genesis, maintenance, and intensity of pain. A comprehensive approach is therefore essential for a more complete understanding and for effective interventions.
Finally, a multidisciplinary team is crucial to reduce therapeutic failures and avoid iatrogenesis that may favor pain chronification [9]. In an integrated manner, it is recommended that dentistry conduct diagnosis, fabrication of occlusal splints, and oral rehabilitation; physiotherapy apply relaxation techniques, electrotherapeutic resources, and therapeutic exercises; psychology provide behavioral interventions and cognitive-behavioral therapy with stress management strategies; speech therapy act in functional reeducation and elimination of parafunctional habits; and neurology participate in the evaluation and management of associated headaches.
The limitations of this review include the fact that the included studies were very different from one another, especially regarding the criteria used to diagnose TMD, the ages evaluated, and the methods used to measure symptoms. Many studies also had small samples and did not use the same assessment instruments, which makes comparison of results difficult. In addition, there are still few studies that follow children over longer periods, which prevents a better understanding of how TMD evolves in this age group. A lack of fully adapted and validated instruments for children was also observed in some studies. Finally, the predominance of cross-sectional studies hinders understanding of the clinical progression of TMD in pediatric age and reinforces the need for prospective and standardized research.
Conclusion
It is observed that the diagnosis of temporomandibular disorders should prioritize the use of criteria adapted to the pediatric age group, such as the DC/TMD, combined with an anamnesis directed toward aspects of sleep and stress, in addition to a careful functional examination. The use of imaging examinations should be reserved only for cases in which there is clinical indication.
With regard to treatment, it is recommended to begin with conservative and interdisciplinary approaches, involving pain and habit education, the use of occlusal splints when indicated, physiotherapy, and cognitive, behavioral, or speech therapy interventions, according to individual needs.
Finally, the importance of public policies aimed at training primary health care professionals is highlighted, in order to promote early screening and the establishment of appropriate referral and care pathways.
References
- Carrara SV, Conti PCR, Barbosa JS (2010) Termo do 1º consenso em disfunção temporomandibular e dor orofacial. Dental Press Journal of Orthodontics. 15: 114-120.
- Clark GT, Tsukiyama Y (2003) Occlusal therapy for temporomandibular disorders: A critical review. Journal of the American Dental Association. 134(6): 757-764.
- Bertoli FMDP, Losso EM, Moresca RC (2009) Disfunção da articulação temporomandibular em crianças. RSBO Revista Sul- Brasileira de Odontologia. 6(1): 77-84.
- Ekbert E, Nilsson IM, Michelotti A, Al-Khotani A, Alstergren P, et al. (2023) Diagnostic Criteria for Temporomandibular Disorders — INfORM recommendations: Comprehensive and short-form adaptations for adolescents. J Oral Rehabil. 50(11): 1167-1180.
- Engel G (1977) The Need for a New Medical Model: A Challenge for Biomedicine. Science. 196(4286): 129-36.
- Finck NS, Pacheco MCT, de Araújo MTM (2025) Association of clinical indicators in TMJ, craniofacial, occlusal, and upper airway changes with symptoms of pediatric obstructive sleep apnea and mouth-breathing. Cranio. 43(5): 802-808.
- Koh H, Robinson PG (2003) Occlusal adjustment for treating and preventing temporomandibular joint disorders. Cochrane Database of Systematic Reviews. 1.
- Minervini G, Franco R, Marrapodi MM, Fiorillo L, Cervino G, et al. (2023) Prevalence of temporomandibular disorders in children and adolescents evaluated with Diagnostic Criteria for Temporomandibular Disorders: A systematic review with meta- analysis. J Oral Rehabil. 50(6): 522-530.
- Porto BA, CavalcanteML, Façanha RC (2024) Tratamento Multidisciplinar das Disfunções Temporomandibulares: Uma Revisão Sistemática De Literatura. Revista de Investigação Biomédica. 14(1).
- Rongo R, Ekberg E, Nilsson IM, Al-Khotani A, Alstergren P, et al. (2022) Diagnostic criteria for temporomandibular disorders in children and adolescents: An international Delphi study Part 2 Development of Axis II. Journal of Oral Rehabilitation. 49(5): 541-552.
- Rongo R, Ekberg EC, Nilsson IM, Al-Khotani A, Alstergren P, et al. (2021) Diagnostic Criteria for Temporomandibular Disorders (DC/TMD) for children and adolescents: An international Delphi study — Part 1: Development of Axis I. J Oral Rehabil. 48(7): 836-45.
- Rosal TDP, Ferreira RB (2019) Disfunção temporomandibular em crianças: como diagnosticar?. R Odontol Planal Cent. 4(1): 1-6.
- de Sena MF, de Mesquita KSF, Santos FRR, Silva FWGP, Serrano KVD (2013) Prevalence of temporomandibular dysfunction in children and adolescents. Revista Paulista De Pediatria. 31(4): 538–545.
- Tapia-Sierra FE, Ticona-Flores JM, Reichard-Monefeldt G, Elvira-Tapia N, Gallardo-López NE, et al. (2025) Manifestações clínicas de distúrbios temporomandibulares e sua relação com distúrbios do sono e distúrbios emocionais em uma população pediátrica espanhola: um estudo transversal. J Clin Med.
- Tsukiyama Y, et al. (2001) The effect of occlusal adjustment on temporomandibular disorders: a systematic review of the literature. Journal of Prosthetic Dentistry. 86(5). 455-460.
- Yost O, Liverman CT (2020) Temporomandibular disorders: priorities for research and care. NIH.