Chukwuemeka Igwe*, Nicholas Watson, Yasir Bakhit, Chika Igwe, Simon Stinchcombe
King’s mill Hospital, Sherwood Forest Hospitals Trust, General hospital in Sutton-in-Ashfield, England, UK
*Corresponding Author: Chukwuemeka Igwe, King’s mill Hospital, Sherwood Forest Hospitals Trust, General hospital in Sutton-in-Ashfield, England, UK.
Abstract
Inverted Meckel's diverticulum is a condition in which the diverticulum inverts itself into the bowel. It needs to be understood how such an inversion occurs due to the condition's rarity. However, some factors contributing to the inversion include abnormal peristalsis around the diverticulum and non-fixity of the diverticulum itself. The inverted diverticulum can cause luminal compromise and act as a lead point for intussusception, leading to obstruction. It is rarely encountered in medical practice.
We present a 34-year-old male who presented multiple times with complaints of recurrent intermittent right-sided abdominal pain of about 2 years duration. He subsequently developed more intense abdominal pain associated with vomiting and poor oral intake. Imaging revealed an ileocolic intussusception with no intestinal obstruction.
Introduction
Inverted Meckel's diverticulum is an intraluminal, blind-ending structure usually at the mid to distal ileum, which occurs due to persistence of the congenital omphalomesenteric duct and incidentally found, or through a clinical evaluation for intestinal obstruction, intussusception, gastrointestinal bleeding, and abdominal pain [1]. Bleeding is the most typical clinical presentation, particularly in younger patients [2]. Inverted Meckel's diverticulum is a rare pathological finding and a rare cause of small bowel obstruction [3]. Computed tomography (CT) remains the diagnostic tool for identifying intestinal obstruction and intussusception cases. The most useful diagnostic tool in patients with bleeding and ectopic gastric mucosa is the technetium-99m pertechnetate scan (Meckel's scan) [4].
Case Presentation
A 34-year-old, previously fit and well, presented multiple times and complained of recurrent intermittent right-sided abdominal pain for about 2 years. Initial examination findings were normal. Subsequently, numerous episodes of vomiting and more intense colicky left lower abdominal pain with tenderness and absent bowel sounds on examination.
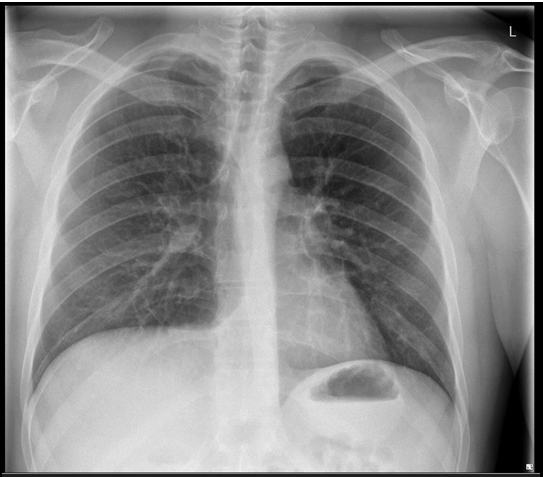
Blood tests were unremarkable, with normal amylase and lactate. Erect Chest X-ray and abdominal X-ray showed no abnormality.
Figure 1: Erect chest X-ray
Figure 2: Abdominal X-ray
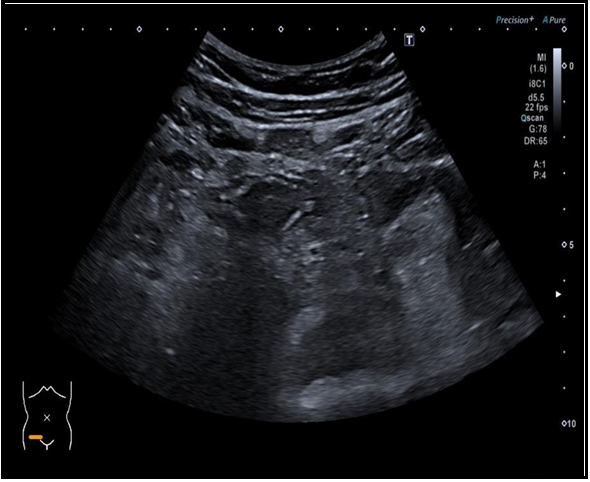
The abdominal ultrasound was unremarkable.
Figure 3: Abdominal ultrasound
The patient had a contrast CT abdomen and pelvis, which showed Ileocolic intussusception with no obstruction, free gas, or free fluid.
Figure 4: Coronal view: Contrast CT Abdomen and Pelvis.
Figure 5: Sagittal view: Contrast CT abdomen and pelvis
Figure 6: Axial view: Contrast CT abdomen and pelvis
The patient did an MRI small bowel study to assess for a possible neoplastic cause, that showed a sizeable pedunculated lesion of fatty signal in the distal small bowel, some distance from the ileocaecal valve, measuring 6 cm in length, which is suggestive of a pedunculated small bowel lipoma. The small bowel was otherwise normal, and no evidence of small bowel obstruction.
Figure 7: Coronal T1: MRI small bowel study
Figure 8: Coronal T2: MRI small bowel study
Figure 9: Coronal T2 Haste: MRI small bowel study
The patient subsequently had a mini-laparotomy with small bowel resection and site-to-site anastomosis, and he did very well post-operation.
Histology of small bowel; macroscopically, measured 185mm length with attached fat measuring up to 32mm. An inverted diverticulum measuring 51mm in length lay 47mm from the nearest longitudinal margin.
The serosa was smooth, and the mucosa around the diverticula was soft and hemorrhagic. On slicing, the diverticulum contained fat.
Sections from the everted diverticulum showed small intestinal mucosa with gastric heterotopia. There was no neoplastic or granulomatous lesion seen. Teams from the rest of the segment of the small intestine were unremarkable. The features were those of the inverted Meckel diverticulum.
Differential Diagnosis
- Inverted appendix
- Intussusception
- Inverted colonic diverticulum
- Lipoma
- Polyp
- Hernia
- Benign or malignant neoplasm.
Discussion
Meckel's diverticulum is an outpouching at the terminal end of the small intestine, which occurs in 1 % - 3 % of the population, making it the most common congenital disability of the gastrointestinal tract5.
It causes symptoms in a tiny population. Most people remain asymptomatic without ever knowing they have Meckel's diverticulum. The disease has an equal male-to-female ratio; however, males are 2-3 times more likely to have complications [6]. Symptoms usually occur in the first year of life but can occur in adults. These will include gastrointestinal bleeding, abdominal pain, cramping, and signs of bowel obstruction (abdominal pain, bloating, diarrhea, constipation, and vomiting). Under 5-year, children have gastrointestinal bleeding as the most typical symptom due to developed ulcers in the small intestine when the diverticulum contains gastric tissues/glands and secretes stomach acid. Bowel obstruction occurs more frequently in older children and adults [6].
Complications which include intussusception, ulceration, stone formation, inflammation, fistulae, small-bowel obstruction, bleeding, perforation, and neoplasm, occur in about 4-40 % of patients with inverted Meckel's diverticulum [2,7].
Diagnosis of inverted Meckel's diverticulum with various imaging modalities is possible. The age at presentation, including different clinical manifestations, is vital for radiologic imaging in making a diagnosis.
Ultrasound is commonplace in pediatric patients and can be helpful in the characterization of inverted Meckel's diverticulum, although of limited value in adults. A hypoechoic blind-ending tubular structure which may be fluid-filled, is seen in the right lower quadrant with the typical gut signature (hyperechoic mucosa), and a connection to the usual small bowel is demonstrable. The echo-free contents are incompressible and inexpressible into the connecting bowel loop8. Enteroliths appear as shadow-producing echogenic foci [9].
Other imaging techniques have mainly replaced barium studies because most cases present acute symptoms. It can demonstrate inverted Meckel's diverticulum as a soft polypoid filling defect located in the distal portion of the ileum10. Masses or ectopic mucosa may cause a filling defect within the diverticulum [11].
Computed tomography (CT) remains the principal modality for identifying intestinal obstruction and intussusception cases. CT can visualize complications such as intussusception, bowel obstruction, and enteroliths. In communication with the small bowel, a blind-ending structure is filled with gas or fluid, mainly when a leading point with intussusception is formed [5,12].
CT enterography has enhanced visualization of the small bowel, hence, higher sensitivity in making a diagnosis [13].
CT angiography may show the persistent omphalomesenteric artery in some individuals with Meckel's diverticulum who present with continued bleeding5. There may be extravasation of contrast material from actively bleeding cases.
Technetium-99m pertechnetate scan has a poor diagnostic value. In this study, gastric mucosa and ectopic gastric tissue take up the pertechnetate, allowing inverted Meckel's diverticulum containing ectopic gastric tissue to be detected5. Hence, other complications, such as intussusception and bowel obstruction, are challenging to diagnose.
Surgical treatment involves segmental resection and anastomosis, which can be done either through open abdominal surgery or laparoscopically.
Conclusion
Inverted Meckel's diverticulum is a rare disease that causes various abdominal symptoms. It occurs because of abnormal peristalsis of the diverticulum due to its non-fixity to the abdomen. Radiologists' and surgeons' attention to this rare clinical entity is essential. Diagnostic assessment is complex due to overlapping clinical and imaging features. However, CT remains the diagnostic tool for identifying intestinal obstruction and intussusception cases. Treatment is by surgery, either through open abdominal surgery or laparoscopically, and includes segmental resection and anastomosis.
Learning Points:
- The radiologist should be friendly with the radiological features of inverted Meckel's diverticulum
- Chronic or recurrent abdominal pain should prompt investigation for possible inverted Meckel's diverticulum
- Radiologic recognition is essential to avoid unnecessary invasive endoscopic investigations and surgical resections to prevent intestinal obstruction.
References
- Elizabeth R, Trevor S, Laura S, Andrew DH (2021) A case report of Meckel's diverticulum. Radiology Case Reports. 16(5): 1118- 1122.
- Sagar J, Kumar V, Shah DK (2006) Meckel's diverticulum: a systematic review. J R Soc Med. 99(10): 501-5.
- Mani VR, Kalabin A, Dinesh A, Rajabalan A, Landa M, et al. (2017) Inverted Meckel's diverticulum: rare etiology of an intestinal obstruction Cureus. 9(10): e1806.
- https://bestpractice.bmj.com/topics/en-gb/804
- Elsayes KM, Menias CO, Harvin HJ, Francis IR (2007) Imaging manifestations of Meckel's diverticulum AJR Am J Roentgenol. 189(1): 81-88.
- Meckel's Diverticulum. Cleveland Clinic.
- Dujardin M, de Beeck BO, Osteaux M (2002) Inverted Meckel's diverticulum a leading point for ileoileal intussusception in an adult: case report, Abdo Imaging. 27(5): 563-565.
- Diverticular disease and fiber. M.A. Eastwood et al., Nutrition & Food Science. 1974.
- Mostbeck GH, Liskutin J, Dorffner R, Bittmann B, Resinger M (2000) Ultrasonographic diagnosis of a bleeding Meckel's diverticulum. Pediatr Radiol. 30(6): 382.
- Hori K, Suzuki Y, Fujimori T (2003) Inverted Meckel’s diverticulum. Surgery. 133(1): 116-117.
- Levy AD, Hobbs CM (2004) From the archives of the AFIP. Meckel diverticulum: radiologic features with pathologic correlation. RadioGraphics. 24(2): 565-587.
- Chong EH, Kim DJ, Kim S, Kim G, Kim WR (2018) Inverted Meckel's diverticulum: Two case reports and a review of the literature. World J Gastrointest Surg. 10(6): 70-74.
- Paulsen SR, Huprich JE, Fletcher JG, Booya F, Young BM, et al. (2006) CT enterography as a diagnostic tool in evaluating small bowel disorders: a review of clinical experience with over 700 cases. Radiographics. 26(3): 641-657.