Alberto Tirelli1, *, Régis Borges Aquino2
¹Anesthesiologist of the São Lucas Hospital (HSL) at the Pontifical Catholic University (PUC), Porto Alegre-RS-Brazil
2Anesthesiologist and Professor in the Department of Anesthesiology of the Medicine Faculty (PUC), Porto Alegre-RS-Brazil
*Corresponding Author: Alberto Tirelli, Anesthesiologist of the São Lucas Hospital (HSL) at the Pontifical Catholic University (PUC), Porto Alegre-RS-Brazil
Abstract
Background and objectives: Madelung’s disease or Multiple Benign Symmetric Lipomatosis, is characterized by symmetric and multiple depositions of fat usually involving the neck and upper chest. For the proposed surgery of mammoplasty by greasy bulky masses, the objective does not use orotracheal intubation due to frequent tracheal involvement of disease 23456 being elected the high thoracic epidural block (HTEB) as anesthetic technique.
Case report: Male patient, with 49 years of age, with 1.58 m and 76 kg with tumor masses in the dorsal region of the trunk, arms, and posterior region of the arms, around the neck, and in the region of the great belt. Smoker for 25 years and report any use of alcohol. HTEB; sitting position, used for skin antisepsis iodized alcohol 70 %, skin anesthesia with lidocaine 1 % (40mg). Tuohy 18 needle puncture at the level of T1 T2 with loss of resistance technique. Injected 50mg ropivacaine solution associated with fentanyl 50mcg and clonidine 30mcg and saline 0.9 % enough to complete total volume of 10 ml, the introduction of an epidural catheter. The surgery lasted 200 minutes and blood pressure (BP) remained around 100/50 mmHg, heart rate (HR) of 70 beats per minute (bpm), and oxygen saturation (Sat) of 99 %. Perioperative sedation with propofol 1 % in infusion. Uneventful post-operative.
Conclusion: The high thoracic epidural blockade proved to be fully satisfactory, as a single technique for mammoplasty surgery of this patient with Madelung's disease and with large peri cervical fat masses. The biggest indication of HTEB is when there is estimate or evidence of difficult orotracheal intubation.
Keywords: Anesthesia, Thoracic Epidural Block, Mammoplasty, Madelung's disease, Systemic Multiple Lipomatosis
Abbreviators: HTEB–High Thoracic Epidural Block; BP–blood pressure; HR–heart rate; BMI-Body Mass Index; CT- Computed
1. Introduction
Madelung's disease has an unknown origin and is linked to chronic alcoholism in 80 % of cases as well as metabolic disorders. Differs from the lipoma of the capsule surrounding the injury. Has as sole treatment liposuction or open surgery for the removal of this fat [1,3]. Can be no recurrence since the fatty cells keep multiplying. First described by Brodie in 1846 as a lipomatous cervical collar. Otto W. Madelung, in 1888, identified 33 patients, and Launois and Bensaude, in 1898, showed 65 cases and for this, it is also known as Launois-Bensaude Syndrome. Its rare occurrence being described little over 200 cases in the world literature [1,3]. Usually comes with dyslipidemia, glucose intolerance, gout, renal tubular acidosis, hyperinsulinemia, and hypolipoproteinemia. The preferred diagnostic exam is computerized tomography or magnetic resonance imaging and histology of the masses of fat [4,8]. There is the Madelung Deformity which is a distal radio dysplasia with deformity, ulnar, and carpal palmar area in the 8 to 12-years old girls [10,11]. There is no relationship with Madelung’s disease known as multiple benign symmetric lipomatosis.
2. Case report
Male patient, with 49 years of age, with 1.58 m and 76 kg. Eight years ago, came watching the growth of tumor masses in the dorsal region of the trunk, arms, and dorsal region of the arms, around the neck and in the region of the great belt. Figures (1) and (2). Smoker for 25 years and report any use of alcohol. Physical exam presenting lucid and coherent and informing with accuracy.
Cardiopulmonary auscultation without peculiarities and opening of the mouth without limitations with Mallampati index III. Blood pressure (BP) 140/90 mmHg, heart rate (HR) 84bpm, BMI = 27 Kg. m-2 laboratory tests: glucose 102mg/dl, estradiol 19.1 pg/ml (5.4 to 65.91), 14.30 ng/ml prolactin (3.7 to 17.9), total testosterone 566 pg/ml (241 to 827) 2 2mUI/ml TSH, LH Miu/ml and 3.8 beta HCG less than 2, 0mUI/ml. In 2008 underwent removal of a greasy mass in the dorsal thoracic region with histopathological indicating atypical lipomatous tumor being diagnosed Madelung’s disease. In the current case, the proposal was bilateral reduction mammoplasty in giant breasts fatty consistency. In the surgical room, monitored with cardio scope, pulse oximeter, and noninvasive blood pressure. Initial data: BP 150/90 mmHg, HR 95 bpm, and (Sat 02) of 100 % in room air. Peripheral venipuncture with a 20 g cannula. Before the HTEB was administered 4 mg EV of midazolam. Placed in a sitting position, used for antisepsis of the skin with a n alcohol-iodine solution to 70 %, skin anesthesia with lidocaine 1 % (40 mg) and 18 Tuohy needle punctures at the level of T1 T2, being injected ropivacaine solution 50 mg, 50 mcg fentanyl-related and clonidine 30mcg and saline 0.9 % enough to complete total volume of 10 ml. This was followed by the introduction of an epidural catheter for 3 cm beyond the tip of the needle. The surgery lasted 200 minutes and the PA remained around 100/50 mmHg, HR of 70 bpm, and 99% of SatO2. Perioperative sedation with propofol 1 % in a continuous infusion, in target concentration of 0.80 mcg/ml, Agília infusion pump of Fresenius Kabi, enough to keep him sedated for the surgery. Post-operative without complications.
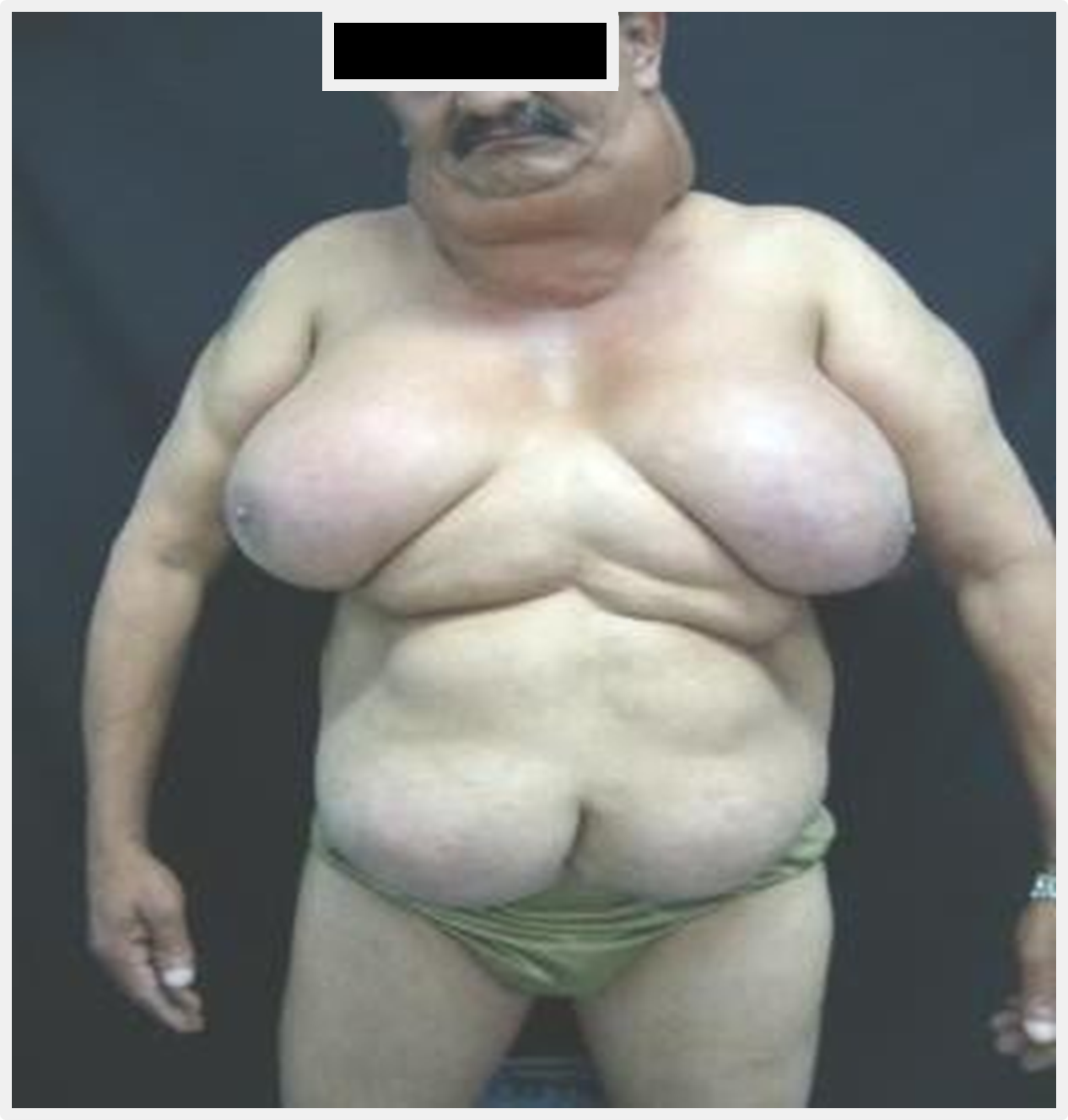
Figure 1: giant breasts
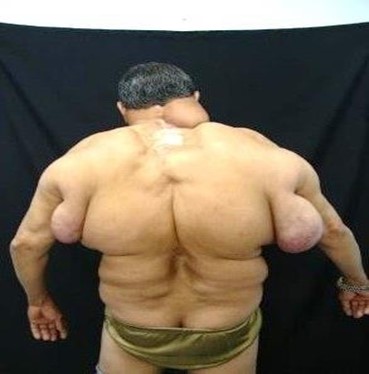
Figure 2: masses in the dorsal region of the trunk
3. Discussion
These lipomatous lesions have features like the absence of an envelope capsule. Hard consistency is due to the fibrous nature and hypervascularity of tissue in addition to deposits of proteoclicanos acids [1,2,6]. The growth of these masses is given by lipomatous cell multiplication, the similarity of neoplasms, and not by hypertrophy of existing cells. This disease is classified into type I lipomatous characterized by deep masses with atrophy of the subcutaneous, in the cervical region, parotid, suprascapular and deltoid’s area. Type II fuzzy-looking distribution of simple obesity. In planning the anesthetic, type I is the highest risk whereas in the cervical region is frequent these hardened masses and accompanied by lymph nodes, causing reactional compressions in digestive tract with dysphagia and breathing tube with dyspnea. [5,7,8]. It is also usual to check for narrowing or deformities in the trachea, larynx, or mediastinum. There are descriptions of tracheal compression, security light observed by cervical CT [2,3,4,5,6]. In some patients the picture of sleep apnea by airway obstruction. In the case of general anesthesia with orotracheal intubation will consider several factors to the success of intubation without injuries. Account the distancing wishbone, distance sternal-cricoid cartilage, Mallampati index, mouth opening, protrusion of Chin, neck mobility, presence of teeth, physician anesthesiologist experience, material available and others. In the case of lipomatosis cervical masses and specifically Madelung disease carriers, several of these predictive are committed negatively and reinforce the degree of difficult intubation. One of the possible alternatives to avoid the airway in these patients, we have the local infiltrative, peripheral blockades and blocks in the neuroaxis. The patient answered was the bearer of great greasy collection at the level of the cervical region and pectoral showing giant breasts. We opted for the HTEB technique (T1 T2) with a catheter for the eventual replacement of volume and doses of anesthetics. Despite the difficulty of spinal tap have been above average, and completion of the epidural block with total success.
4. Conclusion
The thoracic epidural block high proved to be fully satisfactory, as a single technique, for mammoplasty surgery in a patient with Madelung's disease and with large masses of fat peri cervical. HTEB has the biggest indication when there is evidence or estimates of the difficulty of orotracheal intubation.
5. Conflict of interest: None declared.
References
-
GHA Branches, TrevizanGL, Pepe. -Madelung Disease. Rev. Bras. Otorhinolaryngology 2002; 68 (4): 587-90.
-
Marisco PS, seafood GA, AlmeidaAL, Madelung Disease; case report. RJ lung 2010; 19 (1-2); 50-53.
-
Fonseca VAO, Alves C, Marques H, Camacho E, Saraiva AP (2009) Madelung's disease as a rare cause of obstructive sleep apnea. J Bras Pneumol. 35(10); 1053-1056.
-
Vidal M G C, Haygert C J P, Zagoury ET all-AIR Madelung's disease: a case report and literature review. Radiol Bras 2010; 43 (4); 275-76.
-
AC, Bortocello Silva, Bortocello RL ET all RV-Madelung Disease. Case report. Rev. Bras. Clin. Med 2010; 8 (4); 362-4.
-
Teixeira, Kings TG, Bashir AJP ET all. -Lipomatosis benign cervical-Madelung disease. Rev. Bras Cir Cabeça e Pescoço, 2009; 38 (1); 58-59.
-
Yeh CN, CY, Yang Chou CW ET al. -Madelung's Disease. J Clin Endocrinol Met. 2012, 97 (9); 3012- 3013.
-
Rao LP, Manuel EL- Madelung's disease; a case report and literature review. Radiol Bras 2012; 45 (2); 129-31.
-
Sonni VF, Pires CEB, Kay MS ET all. -Madelung Syndrome-case report. Rev. Soc. Bras. Cir. Plástica 1999; 44 (2) 65-74.
-
MO Tachdjian, The neck, and upper limb. Clinical Pediatric Orthopedics: The art of diagnosis and principles of management. Appleton and lange, Stanford, CT 1997 p. 263.
-
Waters PM, The upper limb in Lovell and Winter's Pediatric Orthopaedics, 6th ed. Morrissy RT, Weinstein Sl, ed. Lippincott Williams and wilkins, Philadelphia 2006 p. 921.



