Petar Kiskinov1*, Elean Zanzov1, Kiril Atliev2 Madjit Kadim2, Elena Krasteva1
1Department of Propedeutics of Surgical Diseases; Section of Plastic, Reconstructive and Aesthetic Surgery and Thermal Trauma, Medical University of Plovdiv, Bulgaria
2Department of Urology and General Medicine, *St. George University Hospital, Plovdiv, Bulgaria
*Corresponding Author: Petar Kiskinov, Department of Propedeutics of Surgical Diseases; Section of Plastic, Reconstructive and Aesthetic Surgery and Thermal Trauma, Medical University of Plovdiv, Bulgaria.
Keywords: Complete avulsion, Replantation, Scalp, Trauma, Wound healing
Introduction
A complete scalp avulsion is a rare but serious injury. It is often a life-threatening trauma. Aesthetic problems after the acute period remain a challenge for reconstructive surgery. Apart from the ensuing shock of significant blood loss, the tissue defect is extensive and difficult to reconstruct. The detached part of the scalp may be of different shapes and thicknesses. The most common causes are industrial injuries, animal bites, and criminal activities. Tears usually follow the lines of least resistance: along the insertions of the frontal and temporal muscles anteriorly and the occipital muscle posteriorly. For this reason, the avulsion of entire frontal areas, including browns as well as parts of the ears is common.
In-depth, the tear occurs in the loose connective tissue located between the periosteum of the skull and the galea aponeurotica. Bleeding is usually profuse. According to literature data, it varies between 840ml and 4500ml [1]. It can quickly lead to hemorrhagic shock, so stabilization of the patient before reconstructive treatment is of key importance.
Various reconstructive treatment methods have been described. The "gold standard" nowadays is the technique of free flap microsurgical vascular anastomosis. Due to the lack of adjacent tissues to cover such an extensive defect, microsurgical reconstruction gives very good results, but it is also accompanied by many risks and complications. The first reported case of scalp microvascular replantation was performed by Miller [2] and his team in 1976, as the case presented a successful anastomosis of both temporal arteries and a total of five veins. Cases of successful scalp replantation with anastomosis of only one temporal artery and one vein have been described [3]. In such cases, where microsurgery is not applicable, there is an alternative. Plastic reconstruction with local tissues or free skin grafting in many cases gives good results in covering such extensive defects, although with a less good aesthetic appearance [4].
Material and methods
We present a case of successful scalp replantation without the use of a microsurgical technique. A 32-year-old female patient suffered a work-related accident in which her hair fell into a rotating part of a packaging machine. The result was a total avulsion of the scalp, with torn-off parts of the frontal and temporal muscles, galea aponeurotica, left eyebrow, and the upper 2/3 of the left ear (Figure 1). The patient was transported to the ER department of "St. George" UMHAT, where primary surgical care and hemostasis were performed and the patient was stabilized. Consultations were made with a vascular and plastic surgeon considering possible vascular anastomosis. Because of the severe trauma and multiple tissue lacerations, microsurgical vascular reconstruction was deemed inappropriate. After stabilization of the acute period, treatment continued in the Plastic, reconstructive, and aesthetic surgery clinic in the same hospital, where surgical treatment of the avulsed part began. The hair was removed, along with foreign bodies and devitalized tissue. Until the replantation procedure, the avulsed part was placed in an ice-cold solution of saline and gentamicin. The "warm ischemia" time was about 2 hours and the "cold ischemia" time was about 90 minutes.
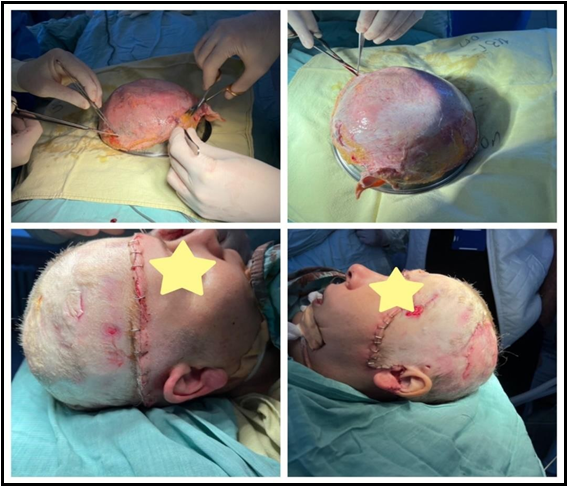
Figure 1: Total scalp with removal of 100 % of hairy skin, frontal, temporal muscles, left eyebrow and ear.
Intraoperative surgical workup continued with vitality assessment followed by thorough debridement of both the avulsed part and the wound surfaces. After treatment of the wound bottom and edges, a process of deglazing the detached part followed. In some areas, an electric dermatome with adjustable cutting thickness was used. After preparation, the process of replanting followed. Single interrupted Vicryl 3/0 and 4/0 sutures as well as surgical staples were used for fixation (Figure 2). Total operative time was 4 hours.
Figure 2: Scalp degreasing and replantation
We observed a smooth postoperative period. On the fourth postoperative day, two small seromas were formed in the parietal areas, which were managed conservatively. On the thirtieth postoperative day, demarcation occurred in the parietal region and at the tip of the left auricle, which necessitated a second operation. The devitalized tissues of the left auricle were removed, and the parietal areas underwent gentle debridement. Conservative therapy was started, consisting mainly of several sessions of hydrotherapy, ointment, and epithelium stimulating dressings. At the end of the third month of treatment, complete epithelialization was achieved (Figure 3). The missing part of the left earlobe is planned to be reconstructed at the next stage.
Figure 3: Results at the end of the treatment
Discussion
The incidence of scalp avulsion trauma is low. Most authors consider the microsurgical anastomosis of scalp avulsion as the first method of choice [3,5,12]. With the technological development in medicine, the frequency of cases treated with microvascular anastomosis is growing. The application of other operative techniques is described in individual cases. The first published material of successful scalp replantation without microsurgery dates back to 1969 and presents a case of a child with avulsion of ¾ hairy part of the head [6].
One of the most important factors in the treatment of scalp avulsion is the time from the incident to the operating room. The viability of avulsed tissue and tolerance to ischemia is debatable [3]. Several authors describe that the skin and subcutaneous tissue tolerate ischemia for approximately 4-6 hours, and this time interval can be increased up to 12 hours, in the condition of significant cooling [7,8]. A case of successful microvascular replantation after nearly 24 hours of ischemia has been described [9]. For this reason, we believe that in any case where we have preservation of the detached part, regardless of the elapsed time, it is appropriate to discuss replantation. Preoperative preparation of scalp avulsion patients and specific tissue processing is extremely important. Antithrombotic prophylaxis with low molecular heparins is mandatory. Thus, the risk of necrotic complications of the avulsed tissue is reduced [10]. Treatment should begin at the accident with temporary hemostasis, volume replacement, analgesia, and cooling of the scalp. In hospital settings, extensive clinical and paraclinical examinations, imaging studies, as well as an interdisciplinary approach to combined traumas are added to the therapy. A microbiological examination of the wound bed is mandatory. In the presence of secretion or inflammatory manifestations postoperatively, the microbial causative agent is isolated and antibiotic treatment is started according to an antibiogram. This reduces the risk of partial or complete loss of the replanted scalp [11].
Tissue replantation has been described as the method of choice for small (<10cm²) and medium tissue defects (10-50cm²) when there is no involvement of cosmetic subunits or areas of permanent hair loss [6]. We support the opinion of several authors [5,12] that the advantages of the microsurgical technique are determined by the restoration of tissue perfusion, achieving a good final aesthetic and functional result. Disadvantages include the need for specific equipment, a prepared team, more complications, and prolonged operative intervention [13]. The operative time in replantation is significantly shorter, but the final result leaves several aesthetic challenges. The created alopecia, a consequence of the removal of hair follicles in the process of degression, is an aesthetic problem with a difficult future solution.
Conclusion
Replantation is a method of treatment of an avulsed scalp with preserved tissues. Regardless of the known shortcomings, the presented case shows an alternative method of choice, in cases where the microsurgical anastomosis is not applicable, with a satisfactory result, aesthetic and functional, in our case satisfying the patient's expectations.
References
- Arashiro K, Ohtsuka H, Ohtani K, Yamamoto M, Nakaoka H, et al. (1995) Entire scalp replantation: case report and review of the literature. J Reconstr Microsurg. 11(4): 245-50.
- Miller GD, Anstee EJ, Snell JA (1976) Successful replantation of an avulsed scalp by microvascular anastomoses. Plast Reconstr Surg. 58(2): 133-6.
- Plant MA, Fialkov J (2010) Total scalp avulsion with microvascular reanastomosis: A case report and literature review. Can J Plast Surg. 18(3): 112-5.
- Anastasova V., Evstatiev D., Zanzov E. Surgical Behavior of Patients with Post-burn Consequences an 8-year Stady Eurasian Union of Scientists 2016; 1: 23-9
- Kalra GS, Goil P, Chakotiya PS (2013) Microsurgical reconstruction of major scalp defects following scalp avulsion. Indian J Plast Surg. 46(3): 486-92.
- Lu MM (1969) Successful replacement of avulsed scalp. Case report. Plast Reconstr Surg. 43(3): 231–234.
- Hung YC, Huang JJ, Hsu CC (2009) Emergency management of total scalp avulsion. Emerg Med J. 26(3): 225-6.
- СЛУЧАИ НА ТЪКАННА РЕПЛАНТАЦИЯ В ОБЛАСТТА НА СКАЛПА- Елеан И. Зънзов, Иван Ж. Трайков, Ваня Н.Анастасова, Атанас И. Баташки*, Станчо С. Проданов, Георги Г. Желев, Елена С. Кръстева
- Sirimaharaj W, Boonpadhanapong T (2001) Scalp replantation: a case report of long ischemic time. J Med Assoc Thai. 84(11): 1629-34.
- Anastasova V, Zanzov E, Krasteva E, Blagoeva V (2022) Thromboembolism after COVID 19 – our experience with 6 cases. Albanian Journal of Trauma and Emergency Surgery. 6(1): 960-967.
- Krasteva E, Anastasova V, Zunzov E (2021) "OUR EXPERIENCE IN DIAGNOSIS AND TREATMENT OF NECROTIZING FASCIITIS." Eurasian Union of Scientists. 5: 14-20.
- Jiang Z, Li S, Cao W (2014) Emergency management of traumatic total scalp avulsion with microsurgical replantation. Ulus Travma Acil Cerrahi Derg. 20(1): 66-70.
- Sabapathy SR, Venkatramani H, Bharathi RR, D'Silva J (2006) Technical considerations in replantation of total scalp avulsions. J Plast Reconstr Aesthet Surg. 59(1): 2-10.